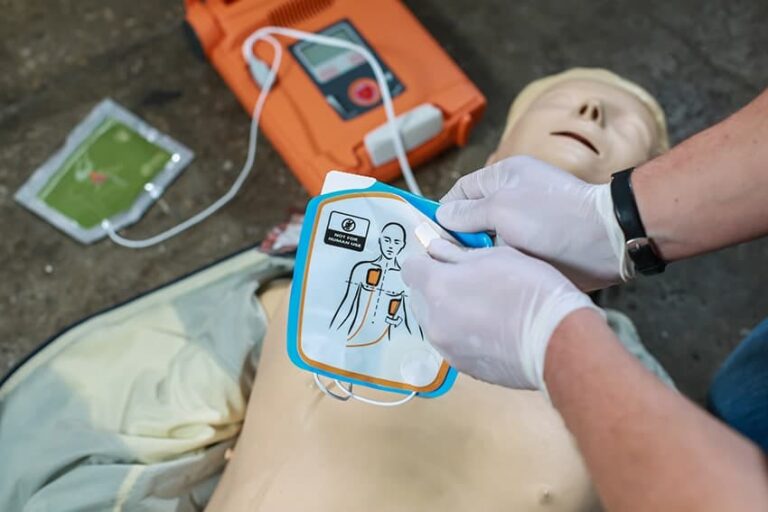
AEDs were originally developed to speed defibrillation in cases of out of-hospital cardiac arrest due to ventricular fibrillation (VF) or pulseless ventricular tachycardia (VT) by enabling more rescuers, including laypeople, to defibrillate.3 The process behind successfully using an AED in an emergency is well-known to healthcare providers and laypersons who have taken even the most basic life-saving courses.
There are some situations that could occur that are outside the “normal” patient care scenario. Some of these situations could be if the patient has a hairy chest, the individual is found in water, the victim has a pacemaker or implantable defibrillator, or the casualty has a medication patch on their chest.
Hairy Chest
For an AED to work properly, the pads must have appropriate contact with the skin. The options to improve conduction with a hairy chest are to either shave the patient with a razor before pad placement, apply significant pressure to the pads to increase conduction, or attach a set of pads and then remove them rapidly in an attempt to remove enough of the hair so the application of new pads will have better placement.1
Patient In Water
The first thing to do if the victim is found in water is to move them to a dry, safe place. If a shock is delivered when the patient is still in water, the shock will be dispersed across the patient’s skin, reducing the effectiveness of the shock, as water is an excellent conductor of electricity.1 The dispersion of electricity is also why the rescuers are not at risk of being shocked.1 An AED can be used safely if the victim is found in a small puddle or in the snow.1 The chest does not need to be completely dry before a shock is delivered, but as much water as possible should be quickly dried from the patient.1
Pacemaker Or Implantable Defibrillator
An internal pacemaker will be surgically placed, usually in the upper aspect of the chest. Current pacemakers are smaller than half a deck of playing cards. AED patches should not be placed over or near the pacemaker. An implantable defibrillator is larger than a pacemaker, approximately the size of full deck of cards, but they are getting smaller. Defibrillators have historically been placed in the abdominal area. AED patches should not be placed that low, but if the defibrillator is seen under the skin higher in the chest, patches should not be placed over the device.1
Medication Patches
Medication patches have been used since the 1970s.2 Some of the medications that can be delivered transdermal are pain medicine, hormones, smoking cessation drugs, nitroglycerin, and many others.1 Used on the skin, transdermal patches may consist of several layers: an adhesive layer that attaches to the skin, a membrane that controls the rate of medication administration, the layer containing the active medication, and the impermeable backing (the visible layer).2 AED patches should not be placed over a medication patch to prevent accidental thermal burns from the delivered shock. If the AED leads need to be placed where a transdermal patch is located, the patch should be removed and the area cleaned to remove all layers and the residual medication on the skin.1
Sources
- American Heart Association. Basic Life Support Provider Manual. 2016;33-40. https://www.nationalcprassociation.com/cpr-aed-study-guide-part-2/.
- Lindauer A, Sexson K, Harvath TA. Teaching caregivers to administer eye drops, transdermal patches, and suppositories. The American Journal of Nursing. 2017;117(5):S11-S16.
- Stewart JA. Automated external defibrillators in the hospital: A case of medical reversal. American Journal of Emergency Medicine. 2017;36:871-874.
Recommended Articles